Bites and stings


IMPORTANT The information provided is of a general nature and should not be used as a substitute for professional advice. If you think you may suffer from an allergic or other disease that requires attention, you should discuss it with your family doctor. The content of the information articles and all illustrations on this website remains the intellectual property of Dr Raymond Mullins and cannot be reproduced without written permission.
Bugs that bite
Mosquitoes and "march flies" can cause nasty itchy bites, but serious allergic reactions are very rare. Ticks also bite, and occasional life-threatening reactions due to tick allergy have been reported. One of the most common causes of severe irritating reactions is from contact with the spines of caterpillars.
Stinging Insects
The Honey Bee is the commonest cause of allergic reactions in Australia overall, but there is regional variability, and the “Jack Jumper” ant is a more common cause of stings in Tasmania. Most bites and stings result in a local itch and swelling that settles within a few days. Native Australian bees and the Green Ant of Queensland can also cause allergic reactions. Unlike honey bees, Paper wasps and European wasps (also know as Yellow Jacket) can sting multiple times, and the latter is particularly aggressive. The "Jumper Ant" is a large black bull-ant prevalent down the eastern side of Australia (Canberra, Snowy River region but also down the south east coast) and Tasmania, as well as the Adelaide Hills and some parts of Western Australia. It is a "hopping" ant, is very aggressive, and can cause severe local pain and sometimes serious allergic reactions. The venoms of these insects are very different. Allergy to one does not increase the risk of reaction to another.
Type of Reactions
Most bites and stings result in a local itch and swelling that settles within a few days. Some will trigger large local swelling that can last for days, and sometimes be mistaken for an infection. More severe allergic reactions can also occur, a condition known as anaphylaxis. Symptoms may include an all-over rash, swelling of tongue or throat, trouble breathing, gut cramps, diarrhoea, vomiting or even a drop in blood pressure. When more severe allergic reactions occur, bees, wasps or "Jumper ants" are usually responsible. Once severe allergy to these insects is established, the tendency to have severe reactions usually persists for over 10 years. The likelihood of serious allergic reactions to mosquito or sandfly bites is close to zero.
Local reactions
Minor Irritant Reactions. Most stinging insects induce minor irritation at the site, which can last hours or days at a time. First Aid measures such as a pain killer, ice, Savlon or a similar antiseptic cream, or an antihistamine tablet (like Claratyne, Lorastyne, Fexotabs, Telfast or Zyrtec) usually suffice.
Moderate Local Reaction. Sometimes the area becomes quite itchy and swollen and can last several days. First Aid measures plus application of a potent cortisone cream under a dressing or plastic wrap can help.
Localised blistering reactions. Development of a localised rash with weeping sores is uncommon, but is managed the same way as for Large Local Reactions (see below).
Large Local Reaction. Swelling can sometimes be severe, and can last up to a week. For example, some people may be stung on a finger, yet the whole hand or arm may swell. It may become hot and red for several days and be mistaken for infection of the bite or sting. These reactions are inflammatory, and may need both antihistamines plus cortisone tablets for a few days. This is a reasonable approach when symptoms are rare, but it is not a good idea to be having lots of cortisone tablets to treat frequent bites and stings. Unfortunately, immunotherapy (desensitisation) is not considered helpful for treatment of these large local reactions and only around 10% ever progress to develop serious allergic reactions.
All over (generalised) reactions
Generalised allergic reactions are usually due to stinging insects like bees, wasps and Jumper ants. The term “generalised” means that the reaction is occurring away from the local sting area. e.g.. all over hives or an acute asthma attack soon after a bee sting. These generalised reactions can be divided into two groups: (a) non-dangerous e.g. hives only, or (b) dangerous. eg. all-over hives, swelling of the tongue or throat, asthma, gut cramps, diarrhoea, vomiting or even a drop in blood pressure resulting in dizziness or loss consciousness. These dangerous reactions can occur within minutes. patients with generalised reactions should be assesses by an allergy specialist, even if symptoms are not dangerous, as even some milder reactions will worsen with time. Those with dangerous reactions (anaphylaxis) usually persists for over 10-15 years, and the risk of recurrent symptoms is approximately 2 out of 3 per sting episode. Clearly, taking tablets that requires an hour to help is inadequate. Adrenaline by injection is the only drug that will work in such a situation.
Important note about local reactions
Even though it is commonly thought that reactions become progressively worse with time, long-term followup studies have shown that less than 1 in 10 large local reactions ever progress to become more serious over time. Stings around the face and neck often cause concern that the throat and tongue will swell too. This is very rare, and as with other localized swellings, takes many hours to develop, giving plenty of time to seek medical assistance if this were to occur. Under normal circumstances, people with local reactions, even when they are large, do not need routine allergy testing, and current practice is that such patients do not need to carry EpiPen/Adrenalineand do not need immunotherapy injections.
Natural History of Allergic Reactions
Local reactions to biting insects like mosquitoes tend to become less severe with time, even if they are very large. Only sometimes do non-dangerous localised allergic reactions become worse, and the outcome is generally better in children than in adults. Unfortunately, serious allergic reactions to stinging insects tend to persist.
Preventing Stings and Bites
1. Bites from midges and mosquitoes are best avoided by covering up as much as possible. Avoid being out doors in the early morning or at dusk, and use a DEET-containing insect repellent like "Rid". Fit insect/fly screens on windows. Remove breeding grounds like ponds and pots from the vicinity. Sometimes area sprays can be used if eating outside in the warmer months, and can be purchased from many supermarkets.
2. Ticks attach themselves to the tips of grass blades, then usually crawl up the inside of clothing to lodge in the head or neck. They are hard to avoid, but wearing socks over long trousers when in the bush and nightly checks for ticks may help. Nightly checks for ticks may help if you live in an endemic area. See additional information on tick allergy.
3. Honey Bees are gentle and normally only sting in self-defence. The best protection is light coloured clothing, covering much of the body (particularly the feet) and avoiding perfume/aftershave.
4. Wasps tend to nest in logs, walls or underground. They are generally more aggressive than bees and attracted to food and drink. Nests are best removed by professionals. The ACT Wasp Hotline is tel 02-6258 5551 if you are aware of European wasp nests that need removal. Please note: the ACT Govt will meet the cost of removal of nests from public land, but removal of nests from private land is at the expense of the property owner. See link: https://www.cityservices.act.gov.au/pets-and-wildlife/wildlife/pest-insects/wasps
5. Don't pretend to be a flower! Avoid bright coloured & black clothing, and don't wear scents. Cover the body (especially the feet) and wear muted colours like white, tan or green. Avoid provoking bees and wasps, have nearby nests removed by professionals, and drive with the windows up and air-conditioner on.
Management of Bites and stings
1. First Aid. Bees usually leave their barbed sting in the skin and die. Flicking the sting out as soon as possible will reduce the amount of venom injected. (By contrast, wasps and bull ants rarely leave their sting in the skin). Cold packs and soothing creams may help.
2. Sometimes oral medicines like antihistamines or steroids are helpful, but they generally take one or more hours to help, might help local reactions but will not prevent the rapid onset of a dangerous allergic reaction.
Patient with life-threatening (anaphylactic) reactions are usually advised to:
1. Seek urgent medical assistance
2. Carry and know how to use injectable adrenaline (EpiPen) to treat severe allergic reactions
3. Undertake a course of immunotherapy (desensitization) injections to "switch off" the allergic reaction over time. This is effective for the treatment of bee and wasp stings. This usually requires a series of injections of purified insect venom, typically 80-100 over a period of 5 years. While there is a vaccine to switch off serious allergic reactions to Jumper ant allergy which has been shown to be affective, it is not commercially available, but research is ongoing. Some centres in Adelaide, Melbourne and Tasmania are able to offer jumper ant immunotherapy but there is not country-wide availability.
Related articles
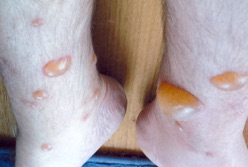
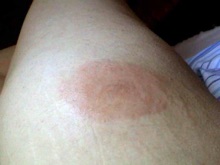
Local reactions to insect bites (left) and sting (right)

Last reviewed 5 June 2020
References
O'Hehir RE, Douglass JA. Stinging insect allergy. Med J Aust 1999; 171: 649-50.
Ford RPK, Dawson KP. Is there a place for bee venom desensitization in children? Aust NZ J Med 1987; 17: 85-91.
Valentine MD et al. The value of immunotherapy with venom in children with allergy to insect stings. N Eng J Med 1990; 323: 1601-3.
Golden DBK et al. Epidemiology of insect venom sensitivity. JAMA 1989; 262: 240-4.
Youlten LJF et al. The incidence and nature of adverse reactions to injection immunotherapy in bee and wasp venom allergy. Clin Exp Allergy 1995; 25: 159-65.
Morris B et al. Effects of stings of Australian native bees. Med J Aust 1988; 149: 707-9.
Clarke PS. The natural history of sensitivity to jack jumper ants (hymenoptera formicidae Myrmecia pilosula) in Tasmania. Med J Aust 1986; 145: 564-6.
Street MD et al. Immediate allergic reactions to Myrmecia ant stings: immunochemical analysis of Myrmecia venoms. Clin Exp Allergy 1994; 24: 590-7.
Van Wye JE et al. IgE antibodies in tick bite induced anaphylaxis. J Allergy Clin Immunol 1991; 88: 968-90.
Solley GO. Allergy to stinging and biting insects in Queensland. Med J Aust 1990; 153: 650-4.
Southcott RV. Some harmful Australian insects. Med J Aust 1988; 149: 656-61.
Reunala T et al. Immunology and treatment of mosquito bites. Clin Exp Allergy 1990; 20: 19-24.
Bellas TE. Occupational inhalant allergy to arthropods. Clinical Reviews in Allergy 1990; 8: 15-29.
Mulvaney JK et al. Lepidopterism: two cases of systemic reactions to the cocoon of a common moth, Chelepteryx collesi. Med J Aust 1998; 168:610-11.
Diwakar L, Noorani S, Huissoon AP, Frew AJ, Krishna MT. Practice of venom immunotherapy in the United Kingdom: a national audit and review of literature. Clin Exp Allergy. 2008 Oct;38(10):1651-8.
Niedoszytko M, de Monchy J, van Doormaal JJ, Jassem E, Oude Elberink JN. Mastocytosis and insect venom allergy: diagnosis, safety and efficacy of venom immunotherapy. Allergy. 2009 Sep;64(9):1237-45.
Bilò BM, Bonifazi F. Epidemiology of insect-venom anaphylaxis. Curr Opin Allergy Clin Immunol. 2008 Aug;8(4):330-7.
Golden DB. Insect sting anaphylaxis. Immunol Allergy Clin North Am. 2007 May;27(2):261-72.
Clark S, Camargo CA Jr. Epidemiology of anaphylaxis. Immunol Allergy Clin North Am. 2007 May;27(2):145-63.
Golden DB. Insect allergy in children. Curr Opin Allergy Clin Immunol. 2006 Aug;6(4):289-93.
Clark S, Camargo CA Jr. Emergency treatment and prevention of insect-sting anaphylaxis. Curr Opin Allergy Clin Immunol. 2006 Aug;6(4):279-83.
Golden DB. Insect sting allergy and venom immunotherapy. Ann Allergy Asthma Immunol. 2006 Feb;96(2 Suppl 1):S16-21.
Greene A, Breisch NL. Avoidance of bee and wasp stings: an entomological perspective. Curr Opin Allergy Clin Immunol. 2005 Aug;5(4):337-41.
Freeman TM. Clinical practice. Hypersensitivity to hymenoptera stings. N Engl J Med. 2004 Nov 4;351(19):1978-84.
Moffitt JE, Golden DB, Reisman RE, Lee R, Nicklas R, Freeman T, deshazo R, Tracy J, Bernstein IL, Blessing-Moore J, Khan DA, Lang DM, Portnoy JM, Schuller DE, Spector SL, Tilles SA. Stinging insect hypersensitivity: a practice parameter update. J Allergy Clin Immunol. 2004 Oct;114(4):869-86.
Brown SG, Heddle RJ. Prevention of anaphylaxis with ant venom immunotherapy. Curr Opin Allergy Clin Immunol. 2003 Dec;3(6):511-6.
Golden DB, Tracy JM, Freeman TM, Hoffman DR; Insect Committee of the American Academy of Allergy, Asthma and Immunology. Negative venom skin test results in patients with histories of systemic reaction to a sting. J Allergy Clin Immunol. 2003 Sep;112(3):495-8.
Golden DB. Discontinuing venom immunotherapy. Curr Opin Allergy Clin Immunol. 2001 Aug;1(4):353-6.
Golden DB, Kagey-Sobotka A, Norman PS, Hamilton RG, Lichtenstein LM. Outcomes of allergy to insect stings in children, with and without venom immunotherapy. N Engl J Med. 2004 Aug 12;351(7):668-74.