Serum sickness

IMPORTANT The information provided is of a general nature and should not be used as a substitute for professional advice. If you think you may suffer from an allergic or other disease that requires attention, you should discuss it with your family doctor. The content of the information articles and all illustrations on this website remains the intellectual property of Dr Raymond Mullins and cannot be reproduced without written permission.
Last reviewed 5 June 2020
Summary
Serum sickness is rare in humans, related to the decrease in usage of foreign serum proteins such as for treatment of snake or spider bite. These days, the most common triggers are medicines.
Introduction
Serum sickness is a relatively rare condition in humans, related to the decrease in usage of foreign serum proteins in treatment of human disease, such as for treatment of snake or spider bite. While these antivenoms and usually produced in horses, it is not known if those with horse allergy have a higher rate of reaction. Similar reactions are seen in response to exposure to a bacterial enzyme called streptokinase (used as a “clot buster” drug) , occasionally with bee stings but most commonly after a course of medication such as antibiotics and more recently, using some monoclonal antibodies for therapeutic reasons.
Mechanism
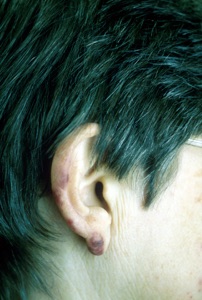
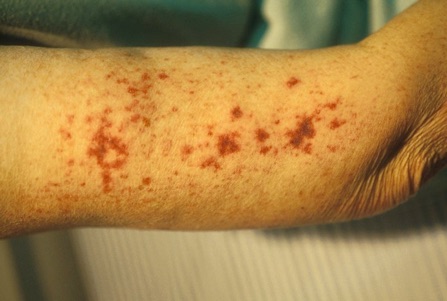
The cause is that the foreign serum, venom or medication in question is recognised as foreign by the immune system This is followed by the generation of proteins called IgG or IgM antibodies, typically 4 - 10 days after initial exposure. As these antibodies bind and interact with the excess foreign "antigen" (foreign serum or medication) circulating immune complexes consisting of antibody and "foreign antigen" are formed and deposited in various organs such as the kidney, skin or joints. Symptoms include flu-like symptoms of fever, itchy hive like and bruising rashes, swelling of the lymph glands or joint swelling and pain can result. Symptoms generally resolve over a period of days or weeks.
Diagnosis
Whilst serum sickness if clearly an immunological reaction, it is not allergic in the strict definition of the word, since IgE antibodies are generally not produced. The implication is that neither RAST testing nor skin testing (which measure IgE) are useful in the confirmation of sensitivity. Diagnosis relies on the recognition of serum sickness as a syndrome, as well as the context in which it occurred. Confirmatory tests such as immune complexes have limited availability in Australia, although measurements of C3 & total haemolytic complement with or without biopsy of suspicious skin lesions are sometimes useful measures.
Management
Serum sickness is usually self limiting and resolves over 2-3 weeks. Treatment with antihistamines, painkillers or even oral cortisone/steroid tablets is sometimes required to hasten recovery and control distressing symptoms.
Other information