Eczema

IMPORTANT The information provided is of a general nature and should not be used as a substitute for professional advice. If you think you may suffer from an allergic or other disease that requires attention, you should discuss it with your family doctor. The content of the information articles and all illustrations on this website remains the intellectual property of Dr Raymond Mullins and cannot be reproduced without written permission.
Summary
Atopic eczema (atopic dermatitis) occurs in around 1 in 5 infants. Symptoms usually improve during the teenage years. Many children either have, or will develop, other allergies with age.
What is eczema?
Atopic eczema occurs in around 1 in 5 infants, but usually improves during the teenage years. Many patients either have or will develop other allergies with age, such as food allergy, hay fever or asthma. Sometimes weeping "sores" may develop as well, particularly if scratched. It usually results in dry, red, scaly and itchy skin. In early childhood, the rash is often present over the face, limbs or trunk. As people get older, it more commonly affects the "creases" such as inside the elbows, behind the knees and in the neck. Like most medical conditions, it can be treated but there is no "cure". Many appear to inherit a defective gene for a protein called called “fillagrin” that help maintain the integrity of the skin; defective protein = defective skin that is less able to withstand environmental irritants.
What makes eczema worse?
Eczema will often have a mind of its own, coming and going without any clear reason. Known aggravating factors include:
-
•Scratching!
-
•Dry skin
-
•Heat
-
•Wool, nylon and acrylic fibres
-
•Sand pits
-
•Viral infections
-
•Teething
-
•Skin infections with the bacteria Staph aureaus
-
•Food allergy
-
•Food irritants e.g. citrus, tomatoes, Vegemite. This is NOT allergy!
-
•Hives / urticaria
-
•Climate changes
-
•Exposure to allergen e.g. dust mite & pets
-
•Other irritants e.g. soap, chlorinated pool water, playing in dirt, grass, bark chips
-
•Stress can make it worse, but eczema is not a psychological condition.
Principles of Therapy
-
•Avoid irritants and known aggravants always
-
•Maintain the protective barrier function of the skin always
-
•Reduce inflammation of eczema with cortisone/steroid lotions when needed
Avoid irritants
Eczema skin has a lower oil and water content than usual and is much easier to irritate than normal skin. Use cotton clothing in children and do not overdress or overheat. "Night gloves" and neatly clipped fingernails will reduce the damage from scratching by youngsters.
Eczema and allergy
Eczema is often called atopic eczema, "allergic" eczema or atopic dermatitis. This is because many either already have other allergies (like hay fever, asthma or food allergy), or will go on to develop them later. The great majority of older patients with eczema are either allergic to dust mite already or become so with time. Direct contact with dust mite droppings ("poo"), animal or grass allergens can be scratched into the skin to worsen the inflammation of eczema.
Food allergy and eczema
Food allergy occurs in around 5 to 10 per cent of very young eczema sufferers, not all patients. It is relatively uncommon in adults with eczema. Food allergy does not cause eczema, but can worsen it. The most common causes are cows milk, soy protein, egg, nuts, seeds, wheat and seafood. Accurate skin testing can be performed, even in young infants and affected babies. The majority of children with food allergy will get obviously intensely itchy with large hives, vomiting and distress within an hour or less of eating, not subtle eczema the nexrt day.
Less commonly, reactions will be delayed over several days. Allergy testing is less reliable in this situation. Fortunately, most food allergies that aggravate eczema will disappear within the first few years of life. Taking young children off wheat and milk as a routine will only help a small proportion of children with eczema, and almost never makes a difference in adults. If it does help, the benefit should be dramatic and noticeable within 1-2 weeks. Long-term unsupervised (and often unnecessary) dietary restriction can lead to malnutrition. Furthermore, there are studies that showing that up to 1 in 10 infants with develop a new food allergy to a previously tolerated food if that food is taken out of the diet.
Not all eczema is allergic
Not all eczema is allergic. Constant exposure to irritants like water, soap, grease, food or chemicals can damage the protective barrier function of the skin. Once the protective barrier of the skin is lost, dermatitis frequently develops.
Good skin care
Hot water washing with excessive use of soap removes skin moisture and worsen the itch. Bathing in warm or tepid water, using a soap substitute or bath oil and liberal application of moisturisers all help to return the skin from a dry, cracked state to an intact barrier that is more resistant to external irritants. There are many brands of moisturiser available. As a rule, it is best to purchase these from a pharmacy / chemist rather than supermarket or health food store, and to avoid perfumed products. Some moisturisers will sting or irritate, particularly broken skin, so it pays to experiment with a range of products to find one that suits. Examples of moisturisers available in Australia include sorbolene, QV lotion, Dermoveen Oatmeal lotion, Aqueous cream, Dermeeze, Alpha Keri lotion and Emulsifying ointment.
IMPORTANT: food is for eating, not for basting in! Do NOT use moisturiser that contains food, and that means anything with nut nut oils or Goats milk soap or moisturiser or topical coconut products. Using topical food on the skin is a great way to induce development of food allergy.
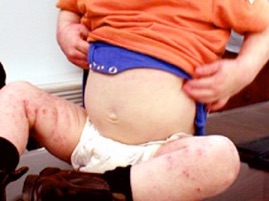
Eczema can get infected
Our skin is covered in bacteria. One of the most common is Staph aureus. Not only can it cause skin infections, but the toxins it releases can also worsen eczema. Infected eczema should be suspected when rashes are very red, raw and angry (not just pink), and when there is a lot of skin oozing of fluid ("weeping eczema"). Mild infections can sometimes be treated with topical antibiotics. Widespread rashes often will need antibiotic tablets or syrups. Frequent infections can be managed by adding antibacterial solutions into the bath, such as Oilatum Plus bath oil, or Ego Flareup oil. Bleach bathes can be of use in the same situation. The ratio is 12ml of 6% household bleach in 10 litres of water. This can be done 1-2/week to reduce the levels of skin Stph bacteria, and reduce the risk of infected eczema. Have a soak for 10 minutes, do not rinse off and dab dry with old towels; you do not want to get beaching of your good towels!
If you do not have a bath, add 1.2ml of bleach into a litre of water and put into a clean spray bottle (get from supermarket). After showering, shake excess water from the body, then spray the dilute bleach over the body. Cloth soaked in the same solution can be applied to the face. Dab dry after 5 minutes; do not rinse off. Then apply topical steroids and moisturiser.
Using cortisone creams wisely
These are applied to inflamed red and itchy areas. They are the only medications that will reduce the inflammation of eczema. They do not cure! The preparations used vary in strength. Your doctor will advise you as to the most suitable preparations for your problem. Shiny skin, thin skin, stretch marks or easy bruising are the major concerns with repeated use. The skin of the face and neck is more sensitive to the side effects of steroid preparations. Directions should be carefully followed to avoid side effects, and creams meant for the body should never be used on the face. Some people find that creams will irritate and sting. Under these circumstances, greasy ointments are often better tolerated. Overall though, more problems with scarring, thickened skin and changes in pigmentation are caused by eczema that is UNDER-treated rather than over-treated. One thus aims for intact skin, using the anti-inflammatory creams until the eczema is gone completely, but to give the cortisone creams 2-3 days off/week to reduce the risk of side-effects.
Newer topical medications
Newer topical medications such as tacrilimus and picrilimus (Elidel) have been developed. These reduce inflammation when applied to the skin. They are not cortisone or steroid-based, but do reduce skin inflammation. They are available by subsidy under certain conditions in Australia, mainly to use on the face.
Other forms of therapy
-
•Cortisone tablets are only rarely used to treat eczema, and even then only for short periods.
-
•Antihistamines are generally of little use in reducing the itch of eczema. Older, drowsy antihistamines sometimes help people sleep through their itch. Sometimes they will help, particularly if the patient has hives (urticaria) as well.
-
•Antibiotics are sometimes necessary when eczema becomes infected.
-
•Immune suppressants are sometimes needed when the inflammation of eczema is very hard to control. They need to be used carefully and under close medical supervision.
-
•Ultraviolet light ("PUVA") reduces inflammation
-
•Relaxation therapy may help when stress pays a role
-
•Evening Primrose Oil, fish oil and flaxseed oil diet supplements are very popular to moisten the skin. Evidence of effectiveness is not that convincing despite testimonials.
-
•Probiotic supplements have gone through a phase of popularity over recent years, but again evidence of benefit is contradictory, so they are not routinely advised as a standard treatment. If they help, the evidence is strongest for reducing the risk of developing eczema if given to pregnant women and their babies rather than in established eczema.
-
•Immunotherapy is only occasionally recommended for the treatment of atopic eczema.
-
•Diet manipulation helps only a minority of patients.
-
•Some patients, mainly with head/neck/shoulder dermatitis have evidence of an allergic response to a skin fungus called Pityrosporum (Malassezia) which may worsen eczema and those affected may improve with topical antifungal treatment.
-
•Vitamin D supplements have been shown to reduce eczema severity in those with low vitamin D levels.
Future Career
Young adults should be advised to seek a career that is less likely to expose them to irritant chemicals or soaps. For example, it is sensible for young adults with on-going eczema to avoid food processing, hairdressing, nursing, catering, the building industry, being a motor mechanic or car repairer. Protective gloves with cotton inner linings are often useful to prevent irritant dermatitis secondary to chemical exposure or maceration from wearing latex or plastic gloves all day (e.g laboratory workers, nurses).
Other information
Australasian Society for Clinical Immunology and Allergy- link
Bleach baths information
Last reviewed 29 May 2020
References
1. Beltrani VS (ed). Atopic dermatitis-an update for the next millenium. J Allergy Clin Immunol 1999; 104: S85-130.
2. Hogan PA. Atopic dermatitis: what to do when the itch becomes too much. Med J Aust 1997; 13-8.
3. Leung DYM. Atopic dermatitis: the skin as a window into the pathogenesis of chronic allergic diseases. J Allergy Clin Immunol 1995; 96: 302-18.
4. Friedmann PS et al. Pathogenesis and management of atopic dermatitis. Clin Exp Allergy 1995; 25: 799-806.
5. Tan BB et al. Double-blind controlled trial of effect of housedust-mite allergn avoidance on atopic dermatitis. Lancet 1996; 347: 15-8.
6. Isolauri E, Turjanmaa K. Combined skin prick and patch testing enhances identification of food allergy in infants with atopic dermatitis. J Allergy Clin Immunol 1996; 97: 9-15.
7. Tanaka M et al. IgE-mediated hypersensitivity and contact sensitivity to multiple environmental allergens in atopic dermatitis. Arch Dermatol 1994; 130: 1393-1401.
8. Joint Task Force on Practice Parameters. Disease management of atopic dermatitis: a practice parameters. Ann Allergy Asthma Immunol 1997; 79:197-211.
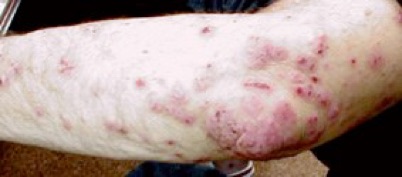
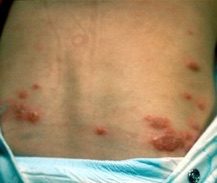
Infected eczema is generally more red, angry in colour and may be weeping liquid.